Understanding how the brain forms and functions from infancy to adulthood.

About Us
The Rutgers Brain Health Institute (BHI) brings together leading researchers to address critical challenges in brain health. Through interdisciplinary collaboration, we aim to translate research into real-world clinical solutions.
Note from Our Director
The Rutgers Brain Health Institute (BHI) serves as the umbrella neuroscience organization across Rutgers University, encompassing over 300 research laboratories and 900 trainees. Our work is organized into four key focus areas: neurodevelopment, neurodegeneration, motivational and affective neuroscience, and cognitive and sensory neuroscience.
Since our inception nearly 10 years ago, BHI has experienced tremendous growth. We have successfully recruited over 35 tenure-track faculty members, with more on the way, and established five Centers of Research Excellence. These include centers dedicated to addiction research, autism research, Alzheimer’s disease research, human neuroimaging, and computational cognitive neuropsychiatry. Additionally, we are in the process of developing new centers focused on pain research and auditory neuroscience.
Our centers reflect our strong translational focus, as we strive to develop innovative approaches to treat brain disorders, including autism, addiction, pain, aging, Alzheimer’s disease, and cognitive disorders like dementia. I invite you to explore our website to learn more about the groundbreaking discoveries that are shaping the future of brain health and advancing our understanding of the human brain—one of the most complex and vital organs.
Thank you,
Gary Aston-Jones, PhD

Bridging Campuses for Impact
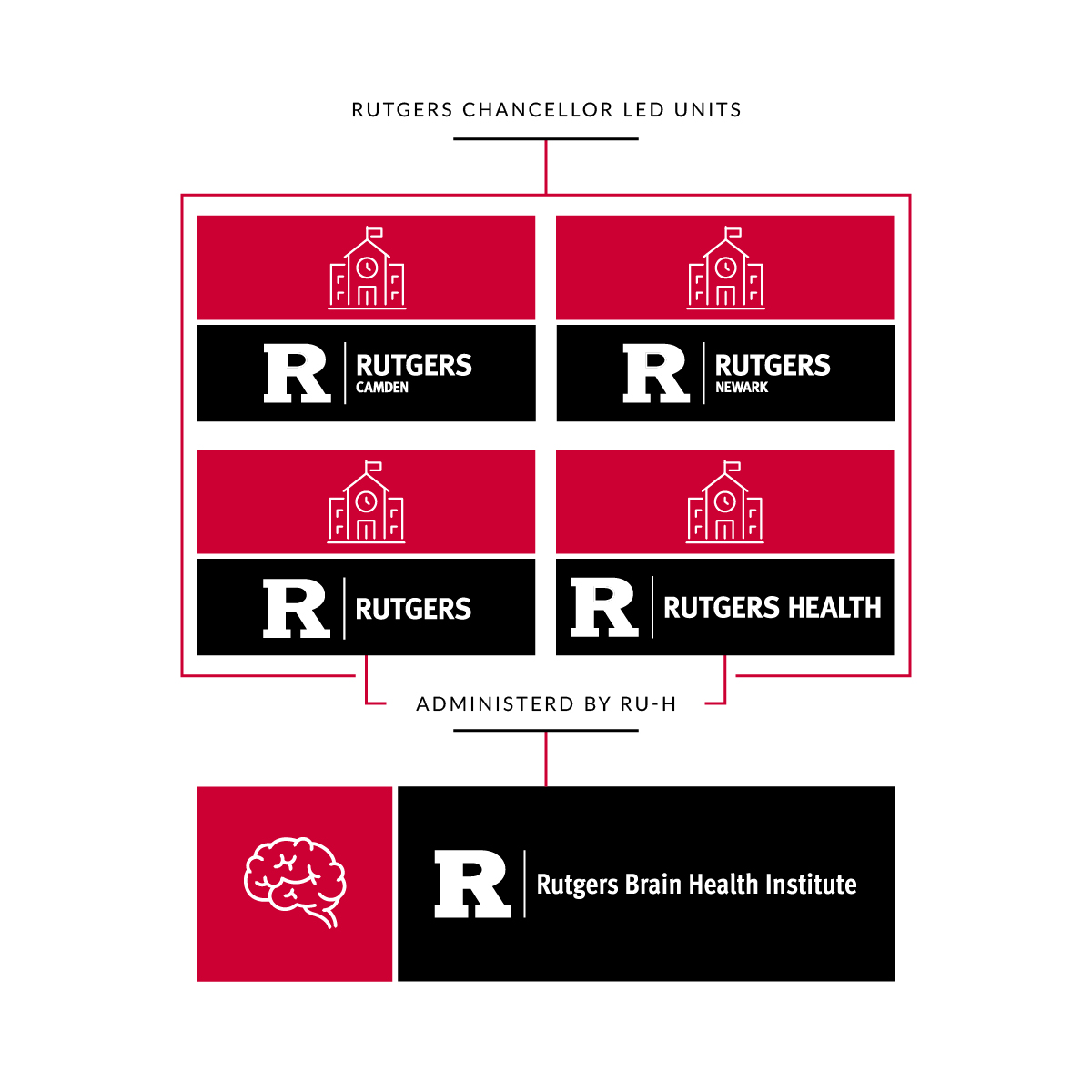
The Brain Health Institute (BHI) is a vital hub that connects the neuroscience community across Rutgers University’s four campuses: Camden, New Brunswick, Newark, and Rutgers Health. By reporting to Rutgers New Brunswick and Rutgers Health, and being administered by Rutgers Health, BHI serves as a unifying entity that fosters collaboration and integration, driving forward advancements in neuroscience research and education.
Diverse Faculty Driving Discovery
At the core of BHI’s mission is its diverse faculty representation, encompassing over 300 members from various disciplines, including Environmental and Biological Sciences, Engineering, Medicine, Social Work, and Public Health. This interdisciplinary expertise enriches our approach to neuroscience and mental health research, creating an environment where innovation and groundbreaking discoveries flourish.

Focused Collaboration for Breakthroughs
To further support this vibrant research community, BHI has established collaborative working groups that focus on critical areas like Neurodegeneration & Injury, Neurodevelopment, Motivational & Affective Neuroscience, and Cognitive & Sensory Neuroscience. These working groups bring together leading experts to address pressing challenges in brain health, while our Postdoctoral Alliance and Junior Faculty Working Groups ensure robust mentorship and professional growth for emerging scientists.

Centers of Research Excellence
Our commitment to advancing neuroscience research is embodied in our Centers of Excellence, which are dedicated to Addiction Research, Autism Research, Alzheimer’s Disease Research, Human Neuroimaging, and Computational Cognitive Neuropsychiatry. These centers serve as pillars of innovation, pushing the boundaries of scientific understanding and developing transformative treatments to improve brain health globally.





Our Vision
Advancing brain health through cutting-edge research

Our Mission
The mission of BHI is to advance brain health through pioneering research, training, and innovation at Rutgers by:
- Promoting multidisciplinary collaborative neuroscience and brain health research.
- Fostering innovative translational studies.
- Cultivating a supportive and inclusive training environment.
- Creating and linking multiple levels of research, from basic discovery through clinical trials.

Our Research Focus
BHI concentrates its efforts in four key areas: Neurodevelopment, Neurodegeneration, Cognitive & Sensory Neuroscience, and Motivational & Affective Neuroscience.
Targeting diseases such as Alzheimer’s and Parkinson’s to find new treatments.
Exploring the mechanisms behind addiction and mental health.
Studying how the brain perceives and processes the world.
Our Community
At BHI, we’re building a vibrant community of researchers, clinicians, students, and supporters.
Together, we’re driving innovation in neuroscience and translating discoveries into meaningful solutions.
Whether you want to collaborate, learn, or support, your involvement makes a difference.